2019 continues to move forward as a year of patient empowerment.
As you may have seen, in August 2018, the Centers for Medicaid and Medicare (CMS) published a final rule for 42 CFR Parts 412, 413, 424, and 495. Now, as with most other goods and services we encounter on a daily basis, cost of care must be made available to consumers in advance of treatment.
This final rule impacts a handful of CMS initiatives—such as interoperability, meaningful use, and quality measures—but leaves an important focus on updating hospital price transparency rules across the inpatient and long-term care hospital prospective payment system (IPPS/LTCH PPS) programs.
The final rule was published in the second half of 2018 and has officially taken effect as of January 1, 2019. By now, in-patient and long-term care hospitals have published their lists of standard charges online. Below is an example of how The Jewish Hospital - Mercy Health has published pricing information on its website:
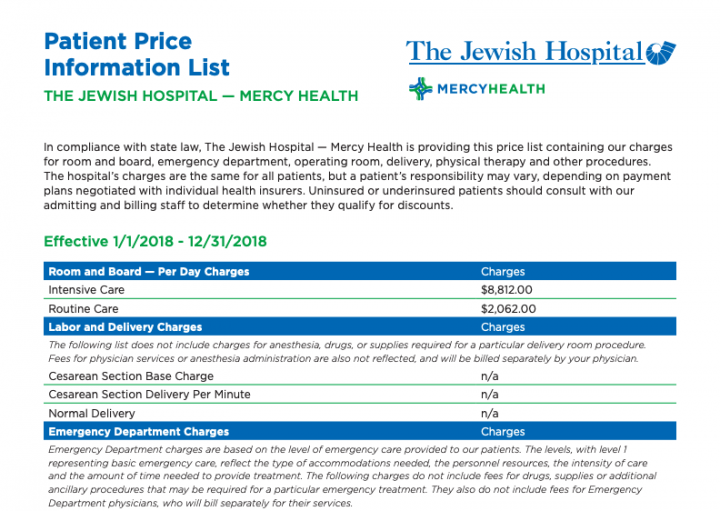
According to the fact sheet released by CMS to accompany these changes, the updates were made to the IPPS and LTCH programs as a way to “further advance the agency’s priority of creating a patient-centered healthcare system by achieving greater price transparency, interoperability, and significant burden reduction so that hospitals can operate with better flexibility and patients have what they need to be active healthcare consumers.”
This is not the first attempt to use healthcare legislation to lower healthcare costs through pricing transparency. In 2008, the Affordable Care Act (ACA) required hospitals to publicize their standard charges for services provided by the hospital. However, the ACA did not specify when, where, or how those charges were published.
Additionally, under the ACA, hospitals only needed to provide their policy for making pricing information available. Under the IPPS/LTCH PPS final rule, requirements are in place to specify how, when, and where pricing lists are published. As of January 1, 2019, lists must be made available online in an accessible, machine-readable format that is required to be manually updated on an annual basis.
While CMS does not outline requirements for hospitals to include care quality information as a part of the new IPPS/LTCH PPS pricing transparency rules, it is encouraged as a way to “help patients understand what their potential financial liability might be for services they obtain at the hospital, and to enable patients to compare charges for similar services across hospitals.” An article from NEJM Catalyst outlined the ultimate goals of CMS, providers, and patients alike for pricing transparency in the chart below.
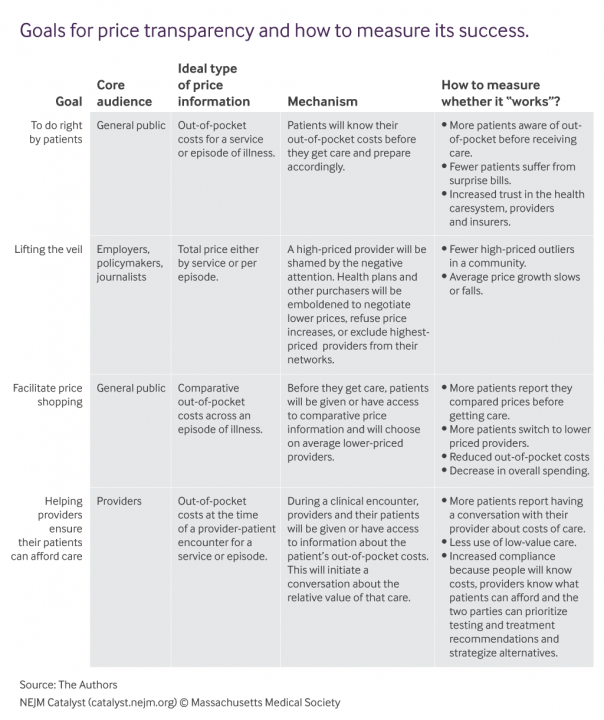
While these changes are clearly intended to improve the overall patient experience, they are not without controversy, with some speculating that providing patients with hospital pricing will not improve the country’s overall healthcare spending. However, pricing transparency has the possibility to leave a major impact by empowering patients with the knowledge to decide when and where they receive care based on how much that care will cost.
Lifting the veil on pricing is an important step forward for patients in healthcare, but it will certainly mean significant changes in how hospitals go about their business. It is in the best interest of most hospitals to develop some strategic messaging to address patient pricing perceptions, limit sticker shock, and push for providers to facilitate pricing conversations with their patients.
Empowering patients to understand all aspects of their health and the care they receive will continue to be an important initiative in 2019. Your organization can support its standard pricing lists by incorporating necessary pricing information in patient onboarding or by adding a patient cost estimate tool to your website. IU Health, a Formstack customer, has implemented a cost estimate tool on its website.
You can easily add a HIPAA-compliant price estimate form to your site today with a free trial from Formstack. Contact our sales team to learn more.





